Are Fallen Arches Flat Feet?
Overview

There are three types of flat feet: flexible flatfoot, painful rigid flatfoot, and spasmodic flatfoot. Flexible flat feet have some arch, even if the arch only appears while the person is flexing the foot or standing on their toes. Flexible flat feet may not cause pain or require treatment. Painful rigid flatfoot, on the other hand, is abnormal and causes pain, stiffness, and the inability to flex the foot. This often indicates that there is a problem with the bones in the foot, a disease is present, or an injury has occurred. Spasmodic flatfoot involves the foot being forced outward by spasmodic contractions of the peroneal muscle.
Causes
There are several reasons why arches fall. It can be genetic, it can be a result of unsupported shoes, a product of our lives and the pressure we put on the feet. Some people have active lifestyles so the wear and tear effect on the muscles there that runs down the back of the calf and wraps around the arch can slacken as we get older. It can be a number of things.
Symptoms
Many people have flat feet and notice no problems and require no treatment. But others may experience the following symptoms, Feet tire easily, painful or achy feet, especially in the areas of the arches and heels, the inside bottom of your feet become swollen, foot movement, such as standing on your toes, is difficult, back and leg pain, If you notice any of these symptoms, it's time for a trip to the doctor.
Diagnosis
Runners are often advised to get a gait analysis to determine what type of foot they have and so what kind of running shoe they require. This shouldn?t stop at runners. Anyone that plays sports could benefit from this assessment. Sports shoes such as football boots, astro trainers and squash trainers often have very poor arch support and so for the 60-80% of us who do overpronate or have flat feet they are left unsupported. A change of footwear or the insertion of arch support insoles or orthotics can make a massive difference to your risk of injury, to general aches and pains and even to your performance.
Can you fix a fallen arch?
Non Surgical Treatment
There are home remedies to prevent or manage pain from fallen arches or flat feet. Here are some areas to consider. Wear footwear or shoe inserts that are appropriate to your activity. When pain occurs, try at-home treatment of rest, ice, and over-the-counter nonsteroidal anti-inflammatories, or NSAIDS, such as ibuprofen. Ask your doctor or a physical therapist to show you stretches that can prepare you for feet-intensive activities. Limit or treat risk factors that can make fallen arches or flat feet worse, such as diabetes, high blood pressure, and obesity. Avoid activities that put excessive stress on your feet, such as running on roads. Avoid high-impact sports such as basketball, hockey, soccer, and tennis. Know when to get help. When pain is severe or interferes with activities, it's time to see the doctor for a thorough exam and treatment.
Surgical Treatment

A combination of surgical procedures can be used to reconstruct the flatfoot. Generally, these procedures can be separated into those that correct deformities of the bones and those that repair ligaments and tendons. Your orthopaedic surgeon will choose the proper combination of procedures for your foot. Surgery of the foot can be performed under regional anesthesia, which is numbing the foot and ankle with a nerve or spinal block, or general anesthesia, which may require a breathing tube. A nerve block is often placed behind the knee to reduce pain after surgery.
Prevention
Sit up straight in a chair with your feet flat on the ground. Scrunch up the toes of one foot as if you are trying to grab hold of the floor then use your toes to drag your foot a small distance forwards. Do this a couple of times on each foot, but don?t use your leg muscles to push your foot forward -- the movement should come solely from the muscles in your feet. Sit in a chair and place a cleaning cloth, towel or small ball on the floor at your feet. Use the toes of one foot to grasp the object and lift it off the floor. This action will require you to clench your toes and contract your arch. Once you have lifted the object a little way off the floor, try to throw it in the air and catch it by stretching your toes and arch out and upwards. Repeat the exercise several times on both feet. Sit on the floor with your legs straight out in front of you then bend your knees out to either side and place the soles of your feet together so your legs form a diamond. Hold on to your ankles and, keeping your heels together at all times, separate your feet so your toes point out to either side. Open and close your feet in this way several times, making sure your little toes stay in contact with the floor throughout the exercise. Starting in the same position, try separating your heels, keeping your toes together at all times.

There are three types of flat feet: flexible flatfoot, painful rigid flatfoot, and spasmodic flatfoot. Flexible flat feet have some arch, even if the arch only appears while the person is flexing the foot or standing on their toes. Flexible flat feet may not cause pain or require treatment. Painful rigid flatfoot, on the other hand, is abnormal and causes pain, stiffness, and the inability to flex the foot. This often indicates that there is a problem with the bones in the foot, a disease is present, or an injury has occurred. Spasmodic flatfoot involves the foot being forced outward by spasmodic contractions of the peroneal muscle.
Causes
There are several reasons why arches fall. It can be genetic, it can be a result of unsupported shoes, a product of our lives and the pressure we put on the feet. Some people have active lifestyles so the wear and tear effect on the muscles there that runs down the back of the calf and wraps around the arch can slacken as we get older. It can be a number of things.
Symptoms
Many people have flat feet and notice no problems and require no treatment. But others may experience the following symptoms, Feet tire easily, painful or achy feet, especially in the areas of the arches and heels, the inside bottom of your feet become swollen, foot movement, such as standing on your toes, is difficult, back and leg pain, If you notice any of these symptoms, it's time for a trip to the doctor.
Diagnosis
Runners are often advised to get a gait analysis to determine what type of foot they have and so what kind of running shoe they require. This shouldn?t stop at runners. Anyone that plays sports could benefit from this assessment. Sports shoes such as football boots, astro trainers and squash trainers often have very poor arch support and so for the 60-80% of us who do overpronate or have flat feet they are left unsupported. A change of footwear or the insertion of arch support insoles or orthotics can make a massive difference to your risk of injury, to general aches and pains and even to your performance.
Can you fix a fallen arch?
Non Surgical Treatment
There are home remedies to prevent or manage pain from fallen arches or flat feet. Here are some areas to consider. Wear footwear or shoe inserts that are appropriate to your activity. When pain occurs, try at-home treatment of rest, ice, and over-the-counter nonsteroidal anti-inflammatories, or NSAIDS, such as ibuprofen. Ask your doctor or a physical therapist to show you stretches that can prepare you for feet-intensive activities. Limit or treat risk factors that can make fallen arches or flat feet worse, such as diabetes, high blood pressure, and obesity. Avoid activities that put excessive stress on your feet, such as running on roads. Avoid high-impact sports such as basketball, hockey, soccer, and tennis. Know when to get help. When pain is severe or interferes with activities, it's time to see the doctor for a thorough exam and treatment.
Surgical Treatment

A combination of surgical procedures can be used to reconstruct the flatfoot. Generally, these procedures can be separated into those that correct deformities of the bones and those that repair ligaments and tendons. Your orthopaedic surgeon will choose the proper combination of procedures for your foot. Surgery of the foot can be performed under regional anesthesia, which is numbing the foot and ankle with a nerve or spinal block, or general anesthesia, which may require a breathing tube. A nerve block is often placed behind the knee to reduce pain after surgery.
Prevention
Sit up straight in a chair with your feet flat on the ground. Scrunch up the toes of one foot as if you are trying to grab hold of the floor then use your toes to drag your foot a small distance forwards. Do this a couple of times on each foot, but don?t use your leg muscles to push your foot forward -- the movement should come solely from the muscles in your feet. Sit in a chair and place a cleaning cloth, towel or small ball on the floor at your feet. Use the toes of one foot to grasp the object and lift it off the floor. This action will require you to clench your toes and contract your arch. Once you have lifted the object a little way off the floor, try to throw it in the air and catch it by stretching your toes and arch out and upwards. Repeat the exercise several times on both feet. Sit on the floor with your legs straight out in front of you then bend your knees out to either side and place the soles of your feet together so your legs form a diamond. Hold on to your ankles and, keeping your heels together at all times, separate your feet so your toes point out to either side. Open and close your feet in this way several times, making sure your little toes stay in contact with the floor throughout the exercise. Starting in the same position, try separating your heels, keeping your toes together at all times.
True Leg Length Discrepancy Test
Overview
Some people have an ?apparent? LLD which may make the affected leg seem longer than the other leg. There are several factors that can contribute to this feeling. Most commonly, contractures or shortening of the muscles surrounding the hip joint and pelvis make the involved leg feel longer, even when both legs are really the same length. Additionally, contractures of the muscles around the lower back from spinal disorders (i.e. arthritis, spinal stenosis), curvatures of the spine from scoliosis, and deformities of the knee or ankle joint can make one leg seem longer or shorter. In the general public, some people have an ?apparent LLD? as long as one half inch but usually don?t notice it because the LLD occurs over time. A ?true? LLD is where one leg is actually longer than the other. Patients can have unequal leg lengths of 1/4? to 1/2? and never feel it too! You can also have combinations of ?True? and ?Apparent? LLDs. During total hip replacement surgery, the surgeon may ?lengthen? the involved leg by stretching the muscles and ligaments that were contracted, as well as by restoring the joint space that had become narrowed from the arthritis. This is usually a necessary part of the surgery because it also provides stability to the new hip joint. Your surgeon takes measurements of your leg lengths on x-ray prior to surgery. Your surgeon always aims for equal leg lengths if at all possible and measures the length of your legs before and during surgery in order to achieve this goal. Occasionally, surgeons may need to lengthen the operable leg to help improve stability and prevent dislocations as well improve the muscle function around the hip.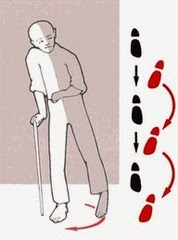
Causes
Leg discrepancy can develop from a medical issue in any portion of the femur or tibia. One leg may lengthen, but leg shortening is much more common. Factors that can cause leg length discrepancy include inherited growth deficiencies. Infections. A bone infection can cause delayed growth in the affected limb. Injury. If your child breaks a leg, it may be shorter once it heals. This is most likely to happen if the fracture or break was complicated, an open fracture, or an injury that affected the growth plate near the end of the bone. Alternatively, a break can cause bones to grow faster after healing, making a leg longer. Tumors. Legg-Calve-Perthes disease. This is a condition that affects the ball (femoral head) of the hip joint. The femoral head may be friable and damage easily, sometimes leading to shortening of the thigh bone. Hemihypertrophy. In children with this condition, one side of the body grows more quickly than the other. Vascular malformations. These are abnormal clusters of veins and arteries that can form close to the bone and stimulate growth. Juvenile arthritis. Inflammation from arthritis can stimulate growth in the affected leg and cause discrepancy.
Symptoms
The symptoms of limb deformity can range from a mild difference in the appearance of a leg or arm to major loss of function of the use of an extremity. For instance, you may notice that your child has a significant limp. If there is deformity in the extremity, the patient may develop arthritis as he or she gets older, especially if the lower extremities are involved. Patients often present due to the appearance of the extremity (it looks different from the other side).
Diagnosis
Leg length discrepancy may be diagnosed during infancy or later in childhood, depending on the cause. Conditions such as hemihypertrophy or hemiatrophy are often diagnosed following standard newborn or infant examinations by a pediatrician, or anatomical asymmetries may be noticed by a child's parents. For young children with hemihypertophy as the cause of their LLD, it is important that they receive an abdominal ultrasound of the kidneys to insure that Wilm's tumor, which can lead to hypertrophy in the leg on the same side, is not present. In older children, LLD is frequently first suspected due to the emergence of a progressive limp, warranting a referral to a pediatric orthopaedic surgeon. The standard workup for LLD is a thorough physical examination, including a series of measurements of the different portions of the lower extremities with the child in various positions, such as sitting and standing. The orthopaedic surgeon will observe the child while walking and performing other simple movements or tasks, such as stepping onto a block. In addition, a number of x-rays of the legs will be taken, so as to make a definitive diagnosis and to assist with identification of the possible etiology (cause) of LLD. Orthopaedic surgeons will compare x-rays of the two legs to the child's age, so as to assess his/her skeletal age and to obtain a baseline for the possibility of excessive growth rate as a cause. A growth chart, which compares leg length to skeletal age, is a simple but essential tool used over time to track the progress of the condition, both before and after treatment. Occasionally, a CT scan or MRI is required to further investigate suspected causes or to get more sophisticated radiological pictures of bone or soft tissue.
Non Surgical Treatment
The object of treatment for leg length discrepancy is to level the pelvis and equalize the length of the two limbs. Inequalities of 2-2.5 centimeters can be handled with the following. Heel lifts/ adjustable heel lifts can be used inside a shoe where shoes have a full heel counter. Heel lifts may be added to the heel on the outside of the shoe along with an internal heel lift. Full platforms along the forefoot and rearfoot area of a shoe can be added. There are many different adjustable heel lifts available on the market. For treatment of a leg length discrepancy, consult your physician. They may refer you to a Physiotherapist or Chiropractor for determination of the type of LLD. A Certified Pedorthist (Canada) will treat a structural leg length discrepancy with a heel lift or in larger discrepancies a footwear modification.

how can we increase our height?
Surgical Treatment
In growing children, legs can be made equal or nearly equal in length with a relatively simple surgical procedure. This procedure slows down the growth of the longer leg at one or two growth sites. Your physician can tell you how much equalization can be gained by this procedure. The procedure is performed under X-ray control through very small incisions in the knee area. This procedure will not cause an immediate correction in length. Instead, the limb length discrepancy will gradually decrease as the opposite extremity continues to grow and "catch up." Timing of the procedure is critical. The goal is to reach equal leg length by the time growth normally ends. This is usually in the mid-to-late teenage years. Disadvantages of this option include the possibility of slight over-correction or under-correction of the limb length discrepancy. In addition, the patient's adult height will be less than if the shorter leg had been lengthened. Correction of significant limb length discrepancy by this method may make a patient's body look slightly disproportionate because of the shorter leg. In some cases the longer leg can be shortened, but a major shortening may weaken the muscles of the leg. In the thighbone (femur), a maximum of 3 inches can be shortened. In the shinbone, a maximum of 2 inches can be shortened.
Some people have an ?apparent? LLD which may make the affected leg seem longer than the other leg. There are several factors that can contribute to this feeling. Most commonly, contractures or shortening of the muscles surrounding the hip joint and pelvis make the involved leg feel longer, even when both legs are really the same length. Additionally, contractures of the muscles around the lower back from spinal disorders (i.e. arthritis, spinal stenosis), curvatures of the spine from scoliosis, and deformities of the knee or ankle joint can make one leg seem longer or shorter. In the general public, some people have an ?apparent LLD? as long as one half inch but usually don?t notice it because the LLD occurs over time. A ?true? LLD is where one leg is actually longer than the other. Patients can have unequal leg lengths of 1/4? to 1/2? and never feel it too! You can also have combinations of ?True? and ?Apparent? LLDs. During total hip replacement surgery, the surgeon may ?lengthen? the involved leg by stretching the muscles and ligaments that were contracted, as well as by restoring the joint space that had become narrowed from the arthritis. This is usually a necessary part of the surgery because it also provides stability to the new hip joint. Your surgeon takes measurements of your leg lengths on x-ray prior to surgery. Your surgeon always aims for equal leg lengths if at all possible and measures the length of your legs before and during surgery in order to achieve this goal. Occasionally, surgeons may need to lengthen the operable leg to help improve stability and prevent dislocations as well improve the muscle function around the hip.

Causes
Leg discrepancy can develop from a medical issue in any portion of the femur or tibia. One leg may lengthen, but leg shortening is much more common. Factors that can cause leg length discrepancy include inherited growth deficiencies. Infections. A bone infection can cause delayed growth in the affected limb. Injury. If your child breaks a leg, it may be shorter once it heals. This is most likely to happen if the fracture or break was complicated, an open fracture, or an injury that affected the growth plate near the end of the bone. Alternatively, a break can cause bones to grow faster after healing, making a leg longer. Tumors. Legg-Calve-Perthes disease. This is a condition that affects the ball (femoral head) of the hip joint. The femoral head may be friable and damage easily, sometimes leading to shortening of the thigh bone. Hemihypertrophy. In children with this condition, one side of the body grows more quickly than the other. Vascular malformations. These are abnormal clusters of veins and arteries that can form close to the bone and stimulate growth. Juvenile arthritis. Inflammation from arthritis can stimulate growth in the affected leg and cause discrepancy.
Symptoms
The symptoms of limb deformity can range from a mild difference in the appearance of a leg or arm to major loss of function of the use of an extremity. For instance, you may notice that your child has a significant limp. If there is deformity in the extremity, the patient may develop arthritis as he or she gets older, especially if the lower extremities are involved. Patients often present due to the appearance of the extremity (it looks different from the other side).
Diagnosis
Leg length discrepancy may be diagnosed during infancy or later in childhood, depending on the cause. Conditions such as hemihypertrophy or hemiatrophy are often diagnosed following standard newborn or infant examinations by a pediatrician, or anatomical asymmetries may be noticed by a child's parents. For young children with hemihypertophy as the cause of their LLD, it is important that they receive an abdominal ultrasound of the kidneys to insure that Wilm's tumor, which can lead to hypertrophy in the leg on the same side, is not present. In older children, LLD is frequently first suspected due to the emergence of a progressive limp, warranting a referral to a pediatric orthopaedic surgeon. The standard workup for LLD is a thorough physical examination, including a series of measurements of the different portions of the lower extremities with the child in various positions, such as sitting and standing. The orthopaedic surgeon will observe the child while walking and performing other simple movements or tasks, such as stepping onto a block. In addition, a number of x-rays of the legs will be taken, so as to make a definitive diagnosis and to assist with identification of the possible etiology (cause) of LLD. Orthopaedic surgeons will compare x-rays of the two legs to the child's age, so as to assess his/her skeletal age and to obtain a baseline for the possibility of excessive growth rate as a cause. A growth chart, which compares leg length to skeletal age, is a simple but essential tool used over time to track the progress of the condition, both before and after treatment. Occasionally, a CT scan or MRI is required to further investigate suspected causes or to get more sophisticated radiological pictures of bone or soft tissue.
Non Surgical Treatment
The object of treatment for leg length discrepancy is to level the pelvis and equalize the length of the two limbs. Inequalities of 2-2.5 centimeters can be handled with the following. Heel lifts/ adjustable heel lifts can be used inside a shoe where shoes have a full heel counter. Heel lifts may be added to the heel on the outside of the shoe along with an internal heel lift. Full platforms along the forefoot and rearfoot area of a shoe can be added. There are many different adjustable heel lifts available on the market. For treatment of a leg length discrepancy, consult your physician. They may refer you to a Physiotherapist or Chiropractor for determination of the type of LLD. A Certified Pedorthist (Canada) will treat a structural leg length discrepancy with a heel lift or in larger discrepancies a footwear modification.

how can we increase our height?
Surgical Treatment
In growing children, legs can be made equal or nearly equal in length with a relatively simple surgical procedure. This procedure slows down the growth of the longer leg at one or two growth sites. Your physician can tell you how much equalization can be gained by this procedure. The procedure is performed under X-ray control through very small incisions in the knee area. This procedure will not cause an immediate correction in length. Instead, the limb length discrepancy will gradually decrease as the opposite extremity continues to grow and "catch up." Timing of the procedure is critical. The goal is to reach equal leg length by the time growth normally ends. This is usually in the mid-to-late teenage years. Disadvantages of this option include the possibility of slight over-correction or under-correction of the limb length discrepancy. In addition, the patient's adult height will be less than if the shorter leg had been lengthened. Correction of significant limb length discrepancy by this method may make a patient's body look slightly disproportionate because of the shorter leg. In some cases the longer leg can be shortened, but a major shortening may weaken the muscles of the leg. In the thighbone (femur), a maximum of 3 inches can be shortened. In the shinbone, a maximum of 2 inches can be shortened.
Understand Heel Pain And Discomfort
Overview

The heel is a cushion of fatty tissue that protects the structures of the foot, including the heel bone, muscles and ligaments. Heel pain is a common foot complaint. Complications include plantar fasciitis and heel spurs. Sever's disease is a common cause of heel pain in children. A podiatrist can help diagnose and treat heel pain. The heel is a padded cushion of fatty tissue around the heel bone (the calcaneus) that holds its shape despite the pressure of body weight and movement. It serves to protect the structures of the foot, including the calcaneus, muscles and ligaments. Heel pain is a very common foot complaint. Anyone can suffer from heel pain, but certain groups seem to be at increased risk, including, middle-aged men and women, physically active people, people who are overweight or obese, people who are on their feet for long periods of time, children aged between eight and 13 years (particularly boys) and women during pregnancy.
Causes
If you have pain behind your heel, you may have inflamed the area where the Achilles tendon inserts into the heel bone (retrocalcaneal bursitis). People often get this by running too much or wearing shoes that rub or cut into the back of the heel. Pain behind the heel may build slowly over time, causing the skin to thicken, become red and swell. You might develop a bump on the back of your heel that feels tender and warm to the touch. The pain might flare up when you first start an activity after resting. It often hurts too much to wear normal shoes. You may need an X-ray to see if you also have a bone spur.
Symptoms
The symptoms of plantar fasciitis include pain along the inside edge of the heel near the arch of the foot. The pain is worse when weight is placed on the foot especially after a long period of rest or inactivity. This is usually most pronounced in the morning when the foot is first placed on the floor. This symptom called first-step pain is typical of plantar fasciitis. Prolonged standing can also increase the painful symptoms. It may feel better after activity but most patients report increased pain by the end of the day. Pressing on this part of the heel causes tenderness. Pulling the toes back toward the face can be very painful.
Diagnosis
After you have described your foot symptoms, your doctor will want to know more details about your pain, your medical history and lifestyle, including. Whether your pain is worse at specific times of the day or after specific activities. Any recent injury to the area. Your medical and orthopedic history, especially any history of diabetes, arthritis or injury to your foot or leg. Your age and occupation. Your recreational activities, including sports and exercise programs. The type of shoes you usually wear, how well they fit, and how frequently you buy a new pair. Your doctor will examine you, including. An evaluation of your gait. While you are barefoot, your doctor will ask you to stand still and to walk in order to evaluate how your foot moves as you walk. An examination of your feet. Your doctor may compare your feet for any differences between them. Then your doctor may examine your painful foot for signs of tenderness, swelling, discoloration, muscle weakness and decreased range of motion. A neurological examination. The nerves and muscles may be evaluated by checking strength, sensation and reflexes. In addition to examining you, your health care professional may want to examine your shoes. Signs of excessive wear in certain parts of a shoe can provide valuable clues to problems in the way you walk and poor bone alignment. Depending on the results of your physical examination, you may need foot X-rays or other diagnostic tests.
Non Surgical Treatment
Treating plantar fasciitis in the early stages usually allows for a quicker recovery. Left untreated, this condition can progress to the point where there is pain with each and every step. This typically means a return to a pain free day will take much longer. Initial treatments are aimed at reducing stress on the fascia so it can begin to heal. Also, treatment to reduce the associated inflammation is started. These treatments often include: ice therapy, anti-inflammatory medications, stretching exercises, wearing shoes with appropriate support, taping of the foot and the use of a night splint. If these interventions do not lead to a full resolution, custom shoe inserts, cortisone injections and additional treatment by a physical therapist are often utilized. For patients that fail to respond to all of these efforts, surgical release of the plantar fascia can be a very effective course of action. The good news is this: 95% of the time plantar fasciitis can be fully resolved without the need for surgery. High energy shock wave therapy, sometimes referred to as orthotripsy, is a relatively new treatment that has been shown to be effective 70% of the time in patients that continue to have pain despite extensive non-surgical treatment.
Surgical Treatment
Although most patients with plantar fasciitis respond to non-surgical treatment, a small percentage of patients may require surgery. If, after several months of non-surgical treatment, you continue to have heel pain, surgery will be considered. Your foot and ankle surgeon will discuss the surgical options with you and determine which approach would be most beneficial for you. No matter what kind of treatment you undergo for plantar fasciitis, the underlying causes that led to this condition may remain. Therefore, you will need to continue with preventive measures. Wearing supportive shoes, stretching, and using custom orthotic devices are the mainstay of long-term treatment for plantar fasciitis.
ankle strap for heels
Prevention

It may not be possible to prevent all cases of heel pain. However, there are some easy steps that you can take to avoid injury to the heel and prevent pain. Whenever possible, you should wear shoes that fit properly and support the foot, wear the right shoes for physical activity, stretch your muscles before exercising, pace yourself during physical activity, maintain a healthy diet, rest when you feel tired or when your muscles ache, maintain a healthy weight.

The heel is a cushion of fatty tissue that protects the structures of the foot, including the heel bone, muscles and ligaments. Heel pain is a common foot complaint. Complications include plantar fasciitis and heel spurs. Sever's disease is a common cause of heel pain in children. A podiatrist can help diagnose and treat heel pain. The heel is a padded cushion of fatty tissue around the heel bone (the calcaneus) that holds its shape despite the pressure of body weight and movement. It serves to protect the structures of the foot, including the calcaneus, muscles and ligaments. Heel pain is a very common foot complaint. Anyone can suffer from heel pain, but certain groups seem to be at increased risk, including, middle-aged men and women, physically active people, people who are overweight or obese, people who are on their feet for long periods of time, children aged between eight and 13 years (particularly boys) and women during pregnancy.
Causes
If you have pain behind your heel, you may have inflamed the area where the Achilles tendon inserts into the heel bone (retrocalcaneal bursitis). People often get this by running too much or wearing shoes that rub or cut into the back of the heel. Pain behind the heel may build slowly over time, causing the skin to thicken, become red and swell. You might develop a bump on the back of your heel that feels tender and warm to the touch. The pain might flare up when you first start an activity after resting. It often hurts too much to wear normal shoes. You may need an X-ray to see if you also have a bone spur.
Symptoms
The symptoms of plantar fasciitis include pain along the inside edge of the heel near the arch of the foot. The pain is worse when weight is placed on the foot especially after a long period of rest or inactivity. This is usually most pronounced in the morning when the foot is first placed on the floor. This symptom called first-step pain is typical of plantar fasciitis. Prolonged standing can also increase the painful symptoms. It may feel better after activity but most patients report increased pain by the end of the day. Pressing on this part of the heel causes tenderness. Pulling the toes back toward the face can be very painful.
Diagnosis
After you have described your foot symptoms, your doctor will want to know more details about your pain, your medical history and lifestyle, including. Whether your pain is worse at specific times of the day or after specific activities. Any recent injury to the area. Your medical and orthopedic history, especially any history of diabetes, arthritis or injury to your foot or leg. Your age and occupation. Your recreational activities, including sports and exercise programs. The type of shoes you usually wear, how well they fit, and how frequently you buy a new pair. Your doctor will examine you, including. An evaluation of your gait. While you are barefoot, your doctor will ask you to stand still and to walk in order to evaluate how your foot moves as you walk. An examination of your feet. Your doctor may compare your feet for any differences between them. Then your doctor may examine your painful foot for signs of tenderness, swelling, discoloration, muscle weakness and decreased range of motion. A neurological examination. The nerves and muscles may be evaluated by checking strength, sensation and reflexes. In addition to examining you, your health care professional may want to examine your shoes. Signs of excessive wear in certain parts of a shoe can provide valuable clues to problems in the way you walk and poor bone alignment. Depending on the results of your physical examination, you may need foot X-rays or other diagnostic tests.
Non Surgical Treatment
Treating plantar fasciitis in the early stages usually allows for a quicker recovery. Left untreated, this condition can progress to the point where there is pain with each and every step. This typically means a return to a pain free day will take much longer. Initial treatments are aimed at reducing stress on the fascia so it can begin to heal. Also, treatment to reduce the associated inflammation is started. These treatments often include: ice therapy, anti-inflammatory medications, stretching exercises, wearing shoes with appropriate support, taping of the foot and the use of a night splint. If these interventions do not lead to a full resolution, custom shoe inserts, cortisone injections and additional treatment by a physical therapist are often utilized. For patients that fail to respond to all of these efforts, surgical release of the plantar fascia can be a very effective course of action. The good news is this: 95% of the time plantar fasciitis can be fully resolved without the need for surgery. High energy shock wave therapy, sometimes referred to as orthotripsy, is a relatively new treatment that has been shown to be effective 70% of the time in patients that continue to have pain despite extensive non-surgical treatment.
Surgical Treatment
Although most patients with plantar fasciitis respond to non-surgical treatment, a small percentage of patients may require surgery. If, after several months of non-surgical treatment, you continue to have heel pain, surgery will be considered. Your foot and ankle surgeon will discuss the surgical options with you and determine which approach would be most beneficial for you. No matter what kind of treatment you undergo for plantar fasciitis, the underlying causes that led to this condition may remain. Therefore, you will need to continue with preventive measures. Wearing supportive shoes, stretching, and using custom orthotic devices are the mainstay of long-term treatment for plantar fasciitis.
ankle strap for heels
Prevention

It may not be possible to prevent all cases of heel pain. However, there are some easy steps that you can take to avoid injury to the heel and prevent pain. Whenever possible, you should wear shoes that fit properly and support the foot, wear the right shoes for physical activity, stretch your muscles before exercising, pace yourself during physical activity, maintain a healthy diet, rest when you feel tired or when your muscles ache, maintain a healthy weight.
What Is Mortons Neuroma
Overview
 Morton?s neuroma is inflammation, thickening, or enlargement of the nerve between the bones of the toes (metatarsal bones). The condition is also called intermetatarsal neuroma. The thickening is usually found between bones of the third and fourth toes of the foot, but sometimes it may develop between the second and third toes. It occurs when the medial plantar nerve near the bones of those toes becomes compressed or irritated, possibly because the metatarsal bones press against the nerve in the narrow gap between the toes. If left untreated, Morton?s neuroma can cause a sharp, burning, or shooting pain that often gets worse over time. The pain becomes worse when a person walks or stands on the ball of the foot. Sometimes the pain reaches the toes next to the neuroma and a sensation of tingling or numbness is felt.
Morton?s neuroma is inflammation, thickening, or enlargement of the nerve between the bones of the toes (metatarsal bones). The condition is also called intermetatarsal neuroma. The thickening is usually found between bones of the third and fourth toes of the foot, but sometimes it may develop between the second and third toes. It occurs when the medial plantar nerve near the bones of those toes becomes compressed or irritated, possibly because the metatarsal bones press against the nerve in the narrow gap between the toes. If left untreated, Morton?s neuroma can cause a sharp, burning, or shooting pain that often gets worse over time. The pain becomes worse when a person walks or stands on the ball of the foot. Sometimes the pain reaches the toes next to the neuroma and a sensation of tingling or numbness is felt.
Causes
Some experts believe that other foot conditions may also be associated with Morton's neuroma. This is because other conditions may cause the metatarsal bones to rub against the nerve in your foot. Foot problems that may increase your risk of developing Morton's neuroma include abnormally positioned toes, high arches, where the arch or instep of your foot is raised more than normal, flat feet, low arches or no arches at all, bunions a bony swelling at the base of the toe. Hammer toe, where the toe is bent at the middle joint. Being active and playing sport can make the painful symptoms of Morton's neuroma worse. In particular, running or sports that involve running, such as racquet sports, can place extra pressure on the nerve in your foot, which can aggravate the problem.
Symptoms
It usually occurs in between the 3rd and 4th toes (about 65% of cases) as is pictured to the right. It is less commonly found in the 2nd webspace, and rarely at all in the 1st or 4th webspaces. You can also experience pins and needles and/or numbness as a result of the nerve being affected. The condition tends to occur predominantly in middle aged females.
Diagnosis
The diagnosis of a Morton's neuroma can usually be made by the doctor when the history of pain suggests it and the examination elicits the symptoms. The foot is generally tender when the involved area is compressed and symptoms of pain and sometimes tingling can be elicited when the sides of the foot are squeezed. Magnetic resonance imaging (MRI) or ultrasound testing can be used to confirm the diagnosis if necessary.
Non Surgical Treatment
Treatment depends on the severity of your symptoms. Your doctor will likely recommend trying conservative approaches first. Arch supports and foot pads fit inside your shoe and help reduce pressure on the nerve. These can be purchased over-the-counter, or your doctor may prescribe a custom-made, individually designed shoe insert, molded to fit the exact contours of your foot.
Surgical Treatment
Surgery to remove the neuroma may be recommended if more conservative treatment does not solve the problem. While surgery usually relieves or completely removes the symptoms, it often leaves a permanent numb feeling at the site of the neuroma.
 Morton?s neuroma is inflammation, thickening, or enlargement of the nerve between the bones of the toes (metatarsal bones). The condition is also called intermetatarsal neuroma. The thickening is usually found between bones of the third and fourth toes of the foot, but sometimes it may develop between the second and third toes. It occurs when the medial plantar nerve near the bones of those toes becomes compressed or irritated, possibly because the metatarsal bones press against the nerve in the narrow gap between the toes. If left untreated, Morton?s neuroma can cause a sharp, burning, or shooting pain that often gets worse over time. The pain becomes worse when a person walks or stands on the ball of the foot. Sometimes the pain reaches the toes next to the neuroma and a sensation of tingling or numbness is felt.
Morton?s neuroma is inflammation, thickening, or enlargement of the nerve between the bones of the toes (metatarsal bones). The condition is also called intermetatarsal neuroma. The thickening is usually found between bones of the third and fourth toes of the foot, but sometimes it may develop between the second and third toes. It occurs when the medial plantar nerve near the bones of those toes becomes compressed or irritated, possibly because the metatarsal bones press against the nerve in the narrow gap between the toes. If left untreated, Morton?s neuroma can cause a sharp, burning, or shooting pain that often gets worse over time. The pain becomes worse when a person walks or stands on the ball of the foot. Sometimes the pain reaches the toes next to the neuroma and a sensation of tingling or numbness is felt.Causes
Some experts believe that other foot conditions may also be associated with Morton's neuroma. This is because other conditions may cause the metatarsal bones to rub against the nerve in your foot. Foot problems that may increase your risk of developing Morton's neuroma include abnormally positioned toes, high arches, where the arch or instep of your foot is raised more than normal, flat feet, low arches or no arches at all, bunions a bony swelling at the base of the toe. Hammer toe, where the toe is bent at the middle joint. Being active and playing sport can make the painful symptoms of Morton's neuroma worse. In particular, running or sports that involve running, such as racquet sports, can place extra pressure on the nerve in your foot, which can aggravate the problem.
Symptoms
It usually occurs in between the 3rd and 4th toes (about 65% of cases) as is pictured to the right. It is less commonly found in the 2nd webspace, and rarely at all in the 1st or 4th webspaces. You can also experience pins and needles and/or numbness as a result of the nerve being affected. The condition tends to occur predominantly in middle aged females.
Diagnosis
The diagnosis of a Morton's neuroma can usually be made by the doctor when the history of pain suggests it and the examination elicits the symptoms. The foot is generally tender when the involved area is compressed and symptoms of pain and sometimes tingling can be elicited when the sides of the foot are squeezed. Magnetic resonance imaging (MRI) or ultrasound testing can be used to confirm the diagnosis if necessary.
Non Surgical Treatment
Treatment depends on the severity of your symptoms. Your doctor will likely recommend trying conservative approaches first. Arch supports and foot pads fit inside your shoe and help reduce pressure on the nerve. These can be purchased over-the-counter, or your doctor may prescribe a custom-made, individually designed shoe insert, molded to fit the exact contours of your foot.

Surgical Treatment
Surgery to remove the neuroma may be recommended if more conservative treatment does not solve the problem. While surgery usually relieves or completely removes the symptoms, it often leaves a permanent numb feeling at the site of the neuroma.
Podiatrists Favor Shoe Lifts For Leg Length Discrepancy
There are two different kinds of leg length discrepancies, congenital and acquired. Congenital indicates that you are born with it. One leg is anatomically shorter in comparison to the other. Through developmental stages of aging, the brain senses the stride pattern and recognizes some variance. The entire body typically adapts by tilting one shoulder to the "short" side. A difference of less than a quarter inch isn't grossly uncommon, does not need Shoe Lifts to compensate and in most cases doesn't have a profound effect over a lifetime.

Leg length inequality goes largely undiscovered on a daily basis, yet this condition is simply corrected, and can eradicate numerous incidents of upper back pain.
Treatment for leg length inequality usually consists of Shoe Lifts. These are typically affordable, usually costing less than twenty dollars, in comparison to a custom orthotic of $200 or even more. When the amount of leg length inequality begins to exceed half an inch, a whole sole lift is generally the better choice than a heel lift. This prevents the foot from being unnecessarily stressed in an abnormal position.
Low back pain is easily the most widespread ailment impacting men and women today. Around 80 million people are afflicted by back pain at some point in their life. It is a problem that costs businesses millions each year as a result of time lost and production. New and better treatment solutions are constantly sought after in the hope of lowering economic influence this issue causes.

People from all corners of the world experience foot ache as a result of leg length discrepancy. In most of these cases Shoe Lifts can be of beneficial. The lifts are capable of alleviating any discomfort in the feet. Shoe Lifts are recommended by many experienced orthopaedic doctors.
To be able to support the human body in a healthy and balanced fashion, the feet have a crucial role to play. In spite of that, it's often the most neglected area of the body. Some people have flat-feet which means there may be unequal force placed on the feet. This will cause other areas of the body like knees, ankles and backs to be impacted too. Shoe Lifts guarantee that appropriate posture and balance are restored.

Leg length inequality goes largely undiscovered on a daily basis, yet this condition is simply corrected, and can eradicate numerous incidents of upper back pain.
Treatment for leg length inequality usually consists of Shoe Lifts. These are typically affordable, usually costing less than twenty dollars, in comparison to a custom orthotic of $200 or even more. When the amount of leg length inequality begins to exceed half an inch, a whole sole lift is generally the better choice than a heel lift. This prevents the foot from being unnecessarily stressed in an abnormal position.
Low back pain is easily the most widespread ailment impacting men and women today. Around 80 million people are afflicted by back pain at some point in their life. It is a problem that costs businesses millions each year as a result of time lost and production. New and better treatment solutions are constantly sought after in the hope of lowering economic influence this issue causes.

People from all corners of the world experience foot ache as a result of leg length discrepancy. In most of these cases Shoe Lifts can be of beneficial. The lifts are capable of alleviating any discomfort in the feet. Shoe Lifts are recommended by many experienced orthopaedic doctors.
To be able to support the human body in a healthy and balanced fashion, the feet have a crucial role to play. In spite of that, it's often the most neglected area of the body. Some people have flat-feet which means there may be unequal force placed on the feet. This will cause other areas of the body like knees, ankles and backs to be impacted too. Shoe Lifts guarantee that appropriate posture and balance are restored.
The Way To Prevent Inferior Calcaneal Spur

Overview
Although a heel spur is often thought to be the source of heel pain, it rarely is. When a patient has plantar fasciitis, the plantar fascia pulls on the bottom of the heel bone. Over time this can cause a spur to form. Heels spurs are a very common x-ray finding, and because the heel spur is buried deep in soft tissue and not truly in a weight bearing area, there is often no history of pain. It is important to note that less than one percent of all heel pain is due to a spur. but frequently caused by the plantar fascia pulling on the heel. Once the plantar fasciitis is properly treated, the heel spur could be a distant memory.
Causes
Athletes who participate in sports that involve a significant amount of jumping and running on hard surfaces are most likely to suffer from heel spurs. Some other risk factors include poor form while walking which can lead to undue stress on the heel and its nerves and ligaments. Shoes that are not properly fitted for the wearer?s feet. Poor arch support in footwear. Being overweight. Occupations that require a lot of standing or walking. Reduced flexibility and the thinning of the fat pad along the bottom of the heel, both of which are a typical depreciation that comes with aging.

Symptoms
Most of the time heel spurs present as pain in the region surrounding the spur, which typically increases in intensity after prolonged periods of rest. Patients may not be able to bear weight on the afflicted heel comfortably. Running, walking, or lifting heavy weight may exacerbate the issue.
Diagnosis
Diagnosis of a heel spur can be done with an x-ray, which will be able to reveal the bony spur. Normally, it occurs where the plantar fascia connects to the heel bone. When the plantar fascia ligament is pulled excessively it begins to pull away from the heel bone. When this excessive pulling occurs, it causes the body to respond by depositing calcium in the injured area, resulting in the formation of the bone spur. The Plantar fascia ligament is a fibrous band of connective tissue running between the heel bone and the ball of the foot. This structure maintains the arch of the foot and distributes weight along the foot as we walk. However, due to the stress that this ligament must endure, it can easily become damaged which commonly occurs along with heel spurs.
Non Surgical Treatment
Initially, treatment usually consists of a combination of ice therapy, stretching exercises to improve flexibility (especially in the mornings), anti-inflammatory medications, and physical therapy. Most patients will also need custom-molded orthotics to help control the motion in the foot and arch, which takes the strain off the plantar fascia. If the pain continues, a cortisone injection may be used to calm the severe swelling and pain. There may the need for a night splint to maintain a stretch in the plantar fascia throughout the night.
Surgical Treatment
Almost 90% of the people suffering from heel spur get better with nonsurgical treatments. However, if the conservative treatments do not help you and you still have pain even after 9 to 12 months, your doctor may advise surgery for treating heel spur. The surgery helps in reducing the pain and improving your mobility. Some of the surgical techniques used by doctors are release of the plantar fascia. Removal of a spur. Before the surgery, the doctor will go for some pre-surgical tests and exams. After the operation, you will need to follow some specific recommendations which may include elevation of the foot, waiting time only after which you can put weight on the foot etc.
What Is The Most Effective Treatment For Heel Spur

Overview
A heel spur is a calcium deposit causing a bony protrusion on the underside of the heel bone. On an X-ray, a heel spur can extend forward by as much as a half-inch. Without visible X-ray evidence, the condition is sometimes known as "heel spur syndrome." Although heel spurs are often painless, they can cause heel pain. They are frequently associated with plantar fasciitis, a painful inflammation of the fibrous band of connective tissue (plantar fascia) that runs along the bottom of the foot and connects the heel bone to the ball of the foot. Treatments for heel spurs and associated conditions include exercise, custom-made orthotics, anti-inflammatory medications, and cortisone injections. If conservative treatments fail, surgery may be necessary.
Causes
A heel spur is caused by chronic plantar fasciitis. Your plantar fascia is a thick fibrous band of connective tissue originating on the bottom surface of the calcaneus (heel bone) and extending along the sole of the foot towards the toes.Your plantar fascia acts as a passive limitation to the over flattening of you arch. When your plantar fascia develops micro tears or becomes inflamed it is known as plantar fasciitis. When plantar fasciitis healing is delayed or injury persists, your body repairs the weak and injured soft tissue with bone. Usually your injured fascia will be healed via fibroblastic activity. They'll operate for at least six weeks. If your injury persists beyond this time, osteoblasts are recruited to the area. Osteoblasts form bone and the end result is bone (or calcification) within the plantar fascia or at the calcaneal insertion. These bone formations are known as heel spurs. This scenario is most common in the traction type injury. The additional bone growth is known as a heel spur or calcaneal spur.

Symptoms
It is important to be aware that heel spurs may or may not cause symptoms. Symptoms are usually related to the plantar fasciitis. You may experience significant pain and it may be worse in the morning when you first wake up or during certain physical activities such as, walking, jogging, or running.
Diagnosis
A Heel Spur diagnosis is made when an X-ray shows a hook of bone protruding from the bottom of the foot at the point where the plantar fascia is attached to the heel bone. The plantar fascia is the thick, connective tissue that runs from the calcaneus (heel bone) to the ball of the foot. This strong and tight tissue helps maintain the arch of the foot. It is also one of the major transmitters of weight across the foot as you walk or run. In other words, tremendous stress is placed on the plantar fascia.
Non Surgical Treatment
Conventional treatment for heel spurs typically includes rest, stretching exercises, icing and anti-inflammatory medications. Many people find it difficult to go through the day without some sort of routine activity or exercise, and this prolongs the heel spur and forces people to rely on anti-inflammatory medications for a longer period of time. This can be detrimental due to the many side effects of these medications, including gastrointestinal problems like leaky gut, bleeding and ulcer symptoms.
Surgical Treatment
Sometimes bone spurs can be surgically removed or an operation to loosen the fascia, called a plantar fascia release can be performed. This surgery is about 80 percent effective in the small group of individuals who do not have relief with conservative treatment, but symptoms may return if preventative measures (wearing proper footwear, shoe inserts, stretching, etc) are not maintained.
Prevention
If you have not yet developed this condition, you can take steps to protect yourself from it. Most importantly, make it a rule to wear properly fitted footwear. Avoid shoes that have become worn down in the heel, and don't choose shoes that cause you to walk in an abnormal fashion. Maintaining a healthy weight will ensure that undue pressure isn't being put on the ligaments, tendons and bones of your feet. If your job requires a great deal of time on your feet, or if you exercise regularly, be sure to balance periods of activity with periods of rest for your feet.